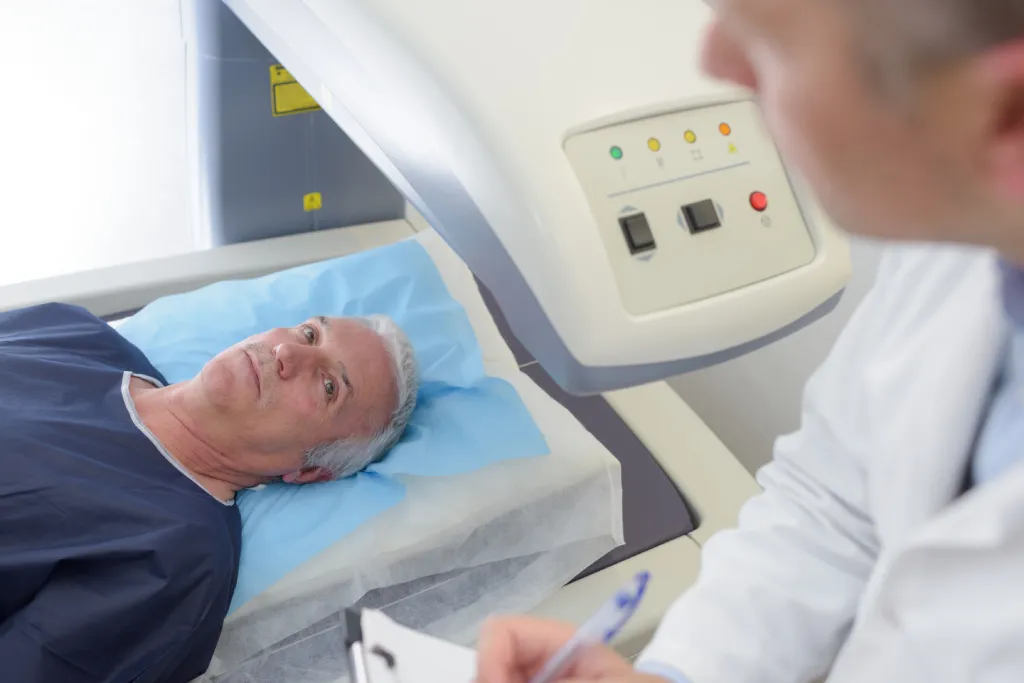
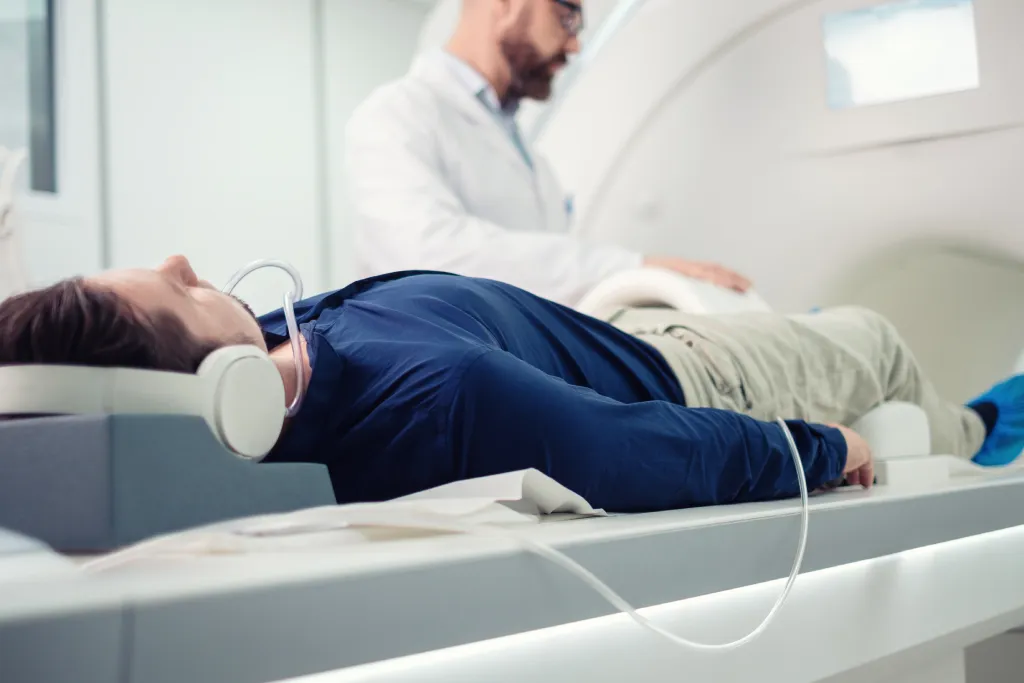
One of our most frequently asked questions is “How accurate is an MRI in detecting prostate cancer?”
Prostate cancer is a prevailing health concern for men, with early detection being paramount to effective treatment and management. As medical technologies evolve, Magnetic Resonance Imaging (MRI) has emerged as a noteworthy tool in the diagnosis of this disease. But how accurate is MRI when it comes to identifying prostate cancer?
Let’s look more closely into the intricacies of prostate cancer, explore the role of MRI in its detection, and evaluate the accuracy and reliability of this imaging technique. Through a comprehensive analysis of research findings, comparison with other diagnostic methods, and insights into future developments, we aim to provide a holistic understanding of the significance of MRI in the battle against prostate cancer.
What is Prostate Cancer?
Prostate cancer is one of the most common types of cancer that affects men. It occurs when cells in the prostate gland, a small walnut-shaped gland that produces seminal fluid, begin to grow uncontrollably. Understanding prostate cancer is critical for early detection and effective management.
As we have discussed on our website, Approximately 1-in-8 men will be diagnosed with prostate cancer in their lifetime. It is the second most common form of cancer in men. While more than half of cases occur in men over age 65, men in their late 40s are not immune to the disease.
Risk factors include
- age
- family history
- race (particularly non-Hispanic black men: 1 in 6 will be diagnosed)
- obesity
Prostate cancer is highly treatable, but research has shown that early screening and accurate diagnosis are key. Early detection and diagnosis improve the chances that a minimally invasive treatment could be a reasonable option for you.
Challenges in Detecting Prostate Cancer
There are several challenges associated with diagnosing prostate cancer, which make it imperative to continuously improve and refine detection methods.
Historically, doctors have questioned the reliability of commonly available screening tests. Many of the concerns break down as follows:
- While PSA tests are commonly used for initial prostate cancer screening, elevated PSA levels are not exclusive to prostate cancer.
- They can be influenced by other factors such as age, prostate infections, and certain medications. This sometimes leads to increased PSA levels without having prostate cancer.
- Digital Rectal Exam (DRE) is limited by the physician’s ability to feel abnormalities and its sensitivity is relatively low for detecting early-stage but clinically significant prostate cancers.
- Biopsies are invasive and come with risks of infection, bleeding, and discomfort. The most common methodology is for a urologist to look at the prostate and divide it into 12 sections and take a needle biopsy sample from each one. Since this is not a targeted approach, the segmental biopsy has a miss rate of about 30-40% in patients with clinically significant prostate cancer. In other words, 30-40% of men who have clinically significant cancer who undergo this traditional biopsy approach will get a negative biopsy result thinking they do not have cancer when in fact they do!
As a means to overcome some of these concerns, MRI has been employed for both the detection of prostate cancer and as a means of guiding a biopsy needle into the cancer.
How Accurate is MRI for Prostate Cancer?
When it comes to diagnostic accuracy, MRI has been found to outperform traditional prostate biopsy. A study published in the Canadian Medical Association Journal found that MRIs are accurate in diagnosing prostate cancer 93% of the time, compared with only 48% for traditional, non-targeted biopsies. While there are a range of factors that might impact those results, they suggest that a high quality MRI is good for detecting prostate cancer.
To improve how accurate a prostate MRI can be in cancer detection and treatment, treatment centers need a high quality MRI, good preparation and scanning protocols, and an expert to read the images. The experts when it comes to using MRI to diagnose cancer are radiologists skilled in reading prostate MRI, not most urologists.
Typically, the process of using an MRI in diagnosing cancer involves several steps:
- A technician will take an MRI.
- A radiologist will evaluate the MRI and determine which areas indicate possible cancer.
- Using the guidance of the MRI, a targeted biopsy of the suspicious areas is performed, and the cells are examined by a pathologist.
- A Gleason Score will be assigned. As we explain on our website, “Physicians use the Gleason Score to help stage the severity of cancer and plan treatment. Tissue that looks healthy is given a lower number, and tissue that looks like cancer is given a higher number. A score of 7 or above usually requires treatment that is more intensive for the purpose of eliminating the presence of cancer.”
At Prostate Laser Center, we firmly believe that incorporating an MRI in the diagnostic process helps in the accurate detection of clinically significant prostate cancer.
Seeking treatment options for prostate cancer or BPH? Request a consultation today.
NOTE: The information provided on this website is general medical information and does not establish a physician-patient relationship. Please discuss your particular situation with a qualified medical professional.